Posted By Dr Nikhil Puri | Best plastic surgeon in lucknow
Introduction: Artificial Skin Is Powerful — But It’s Often Misunderstood
Artificial skin surgery sits at the intersection of plastic surgery, regenerative medicine, and tissue engineering.
Most public discussions simplify it.
They make it sound like doctors simply “grow new skin in a lab” and place it onto the body. Problem solved.
In reality, artificial skin is usually not a full skin replacement.
It’s more like a biological framework that helps the body rebuild damaged tissue.
Plastic surgeons use it when the body’s natural repair mechanisms are no longer enough.
That usually happens in cases like:
-
severe burns
-
traumatic skin loss
-
chronic wounds
-
reconstructive surgery after tumor removal
-
complex scar reconstruction
But here’s the truth many articles avoid:
Artificial skin works incredibly well in the right conditions, and fails quietly in the wrong ones.
Understanding those conditions is what separates good outcomes from disappointing ones.
Why Artificial Skin Exists in Modern Plastic Surgery
Human skin can regenerate surprisingly well.
Small wounds close quickly. Even moderate injuries can heal with minimal intervention.
But the body struggles when deep dermal layers are destroyed.
The dermis is where the skin’s structural system lives:
-
collagen networks
-
blood vessels
-
fibroblasts
-
regenerative signaling pathways
When this layer is lost, healing becomes chaotic.
Instead of rebuilding healthy skin, the body often produces:
-
dense scar tissue
-
contractures
-
unstable wound coverage
Artificial skin was developed to solve a very specific problem:
the body can regenerate cells, but it struggles to rebuild architecture.
Artificial dermal substitutes provide that missing structure.
They act as a temporary scaffold that guides regeneration.
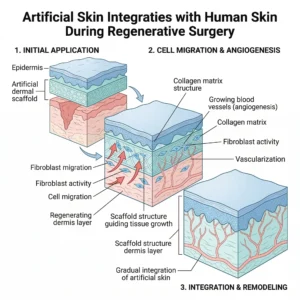
How Artificial Skin Actually Works in Surgery
Most artificial skin products used in plastic surgery have two functional layers.
1. Dermal Scaffold Layer
This layer is usually made from materials like:
-
collagen matrices
-
extracellular matrix proteins
-
biodegradable polymers
-
biologic tissue scaffolds
Its job is to:
-
support fibroblast migration
-
allow new blood vessels to grow
-
guide collagen organization
-
rebuild dermal thickness
Without this structure, regenerated tissue becomes thin and unstable.
2. Temporary Epidermal Barrier
The outer layer often uses silicone or synthetic materials.
This barrier:
-
protects the wound
-
prevents dehydration
-
blocks bacterial contamination
-
mimics the function of the epidermis temporarily
Once the dermal layer integrates, surgeons often place a thin skin graft over it.
So artificial skin is typically one stage in a multi-stage reconstruction process.
Where Artificial Skin Is Most Commonly Used
Artificial skin is not used for every wound.
Surgeons reserve it for situations where traditional grafting alone produces poor results.
Severe Burn Reconstruction
Burns that destroy both the epidermis and dermis leave the body without its natural regenerative template.
Traditional skin grafts in these cases can lead to:
-
stiff scars
-
contractures
-
reduced mobility
Artificial dermal matrices help rebuild dermal thickness, which improves:
-
flexibility
-
graft survival
-
long-term cosmetic outcomes
However, timing is critical.
Apply too early and infection risk increases.
Apply too late and scar formation may already be underway.
Traumatic Skin Loss
Industrial injuries, road accidents, and high-energy trauma can remove large sections of skin.
These wounds often have:
-
irregular wound beds
-
exposed tendons or bone
-
poor tissue support
Artificial skin can stabilize the area and prepare the wound for later grafting.
But trauma wounds frequently carry bacterial contamination, which complicates scaffold integration.
Chronic Non-Healing Wounds
Artificial skin can also help treat wounds that refuse to heal, including:
-
diabetic ulcers
-
pressure ulcers
-
vascular wounds
These wounds fail because the healing environment is disrupted.
Artificial skin provides structural signals that encourage:
-
cell migration
-
vascularization
-
extracellular matrix rebuilding
But success depends heavily on controlling the underlying disease.
If circulation or glucose control remains poor, the treatment may fail.
Artificial Skin vs Traditional Skin Grafts
| Factor | Artificial Skin | Traditional Skin Graft | When Each Is Preferred |
|---|---|---|---|
| Healing Time | Longer initial process due to staged reconstruction | Faster immediate coverage | Grafts for simple wounds |
| Surgical Complexity | Often requires multiple procedures | Single procedure in many cases | Artificial skin for complex wounds |
| Scar Quality | Usually better dermal structure and flexibility | Higher risk of contracture | Artificial skin for functional areas |
| Infection Risk | Higher if wound bed preparation is poor | Lower if graft placed quickly | Grafts in clean wounds |
| Cost | Higher due to advanced materials | Lower surgical cost | Artificial skin for major reconstruction |
| Procedures Required | Often 2 stages (scaffold + graft) | Often 1 procedure | Depends on wound depth |
This comparison shows why artificial skin is not automatically the better choice.
It’s a specialized tool for specific situations.
What Most Articles Don’t Explain
Many discussions about artificial skin focus on innovation.
Few talk about the real-world problems surgeons face.
Three issues come up repeatedly in clinical practice.
Advanced Reality #1: Artificial Skin Can Fail Quietly
Failure rarely looks dramatic.
Instead of obvious rejection, surgeons may see:
-
delayed healing
-
partial integration
-
fragile tissue formation
The scaffold may appear to integrate at first.
But weeks later the regenerated dermis may be thin, weak, or unstable.
This often happens when:
-
bacterial contamination disrupts remodeling
-
inflammation remains elevated
-
blood vessel growth is insufficient
These failures are subtle but important.
Advanced Reality #2: Blood Supply Determines Everything
Artificial skin depends heavily on vascularization.
New blood vessels must grow into the scaffold quickly.
Without adequate blood supply:
-
cells cannot survive
-
nutrients cannot reach the tissue
-
integration fails
Surgeons carefully evaluate wound beds before applying artificial skin.
They look for:
-
healthy bleeding tissue
-
adequate oxygenation
-
strong capillary networks
If vascular support is weak, artificial skin may not work.
Advanced Reality #3: Mechanical Skin Behavior Changes
Even successful regeneration may produce skin that behaves differently.
Artificial dermal structures sometimes produce tissue that is:
-
slightly stiffer
-
less elastic
-
mechanically different from surrounding skin
This becomes important in high-motion areas such as:
-
joints
-
neck
-
eyelids
-
hands
Over time these areas may develop secondary contractures.
Additional reconstructive procedures may be required.
Long-Term Outcomes Surgeons Watch Carefully
Initial healing is only part of the story.
Artificial skin outcomes are evaluated over months or years.
Surgeons monitor for:
-
hypertrophic scars
-
pigmentation differences
-
dermal thinning
-
mechanical instability
Skin experiences constant stress.
If collagen organization within the regenerated dermis is imperfect, problems may appear later.
This is why long-term follow-up is critical.
Future Directions in Artificial Skin Technology
Research is pushing the field toward more advanced solutions.
3D Bioprinted Skin
Scientists are experimenting with printing layered skin structures that include:
-
dermal cells
-
epidermal layers
-
microvascular networks
The goal is to produce skin that behaves closer to natural tissue.
Stem Cell–Based Skin Regeneration
Stem cell technologies may allow surgeons to generate skin using the patient’s own cells.
Potential advantages include:
-
better integration
-
lower immune response
-
improved regenerative signaling
However, clinical implementation remains limited.
Smart Biomaterials
Next-generation scaffolds are being designed to respond to biological signals.
They may release molecules that:
-
reduce inflammation
-
encourage vascular growth
-
guide collagen organization
These materials attempt to solve the biggest limitation today:
slow or incomplete vascularization.
Final Thoughts: Artificial Skin Is a Tool — Not a Miracle
Artificial skin has transformed reconstructive plastic surgery.
It allows surgeons to repair wounds that previously led to severe scarring or disability.
But it is not a universal solution.
Its success depends on:
-
proper wound preparation
-
adequate blood supply
-
infection control
-
thoughtful surgical planning
When these factors align, artificial skin can help the body rebuild tissue that would otherwise heal poorly.
When they don’t, even the most advanced biomaterial cannot overcome biological limitations.
In the end, artificial skin is most powerful when used with careful surgical judgment and realistic expectations.


